Passive EEG-Guided Neuromodulation in Chronic Migraine: Executive Summary
Study Overview
This prospective feasibility study evaluated the Neurogen Brain Balancing Migraine Protocol (NGBBMP), a passive, EEG-guided neuromodulation approach for chronic migraine treatment. Twenty adults (19 female, 1 male; mean age 40.5 years) with an average 14-year migraine history completed five standardized 30-minute sessions over four weeks, delivered by Certified Neurogen Practitioners across multiple U.S. locations and Amsterdam.
Clinical Rationale
Chronic migraine affects approximately 39 million Americans and ranks as the second most disabling condition globally among all ages. Despite widespread pharmacological treatments, up to 40% of patients discontinue preventive medications due to inefficacy or intolerable side effects, with many experiencing only 30-50% reduction in monthly headache days. Traditional neurofeedback, while promising, requires 30-40 sessions over 3-5 months with highly variable outcomes—a burden particularly challenging for migraine sufferers experiencing cognitive fog, sensory sensitivities, and pain.
NGBBMP represents a fundamentally different approach: it is entirely passive, requiring no cognitive effort or behavioral engagement. Using ultra-low-intensity pulsed transcranial electrical signaling (LIP-tES) guided by real-time EEG monitoring, the system detects dysregulated brainwave patterns and applies corrective microcurrents below perceptual thresholds to interrupt maladaptive electrical activity and promote neuroplastic reorganization.
Mechanism of Action
The intervention targets migraine's core neurobiological disturbances:
- Cortical Hyperexcitability: Reduces excessive neuronal firing in sensory cortices
- Thalamocortical Dysrhythmia: Restores rhythmic communication between thalamus and cortex
- Central Sensitization: Interrupts amplified pain processing pathways
- Neuroinflammation: Attenuates inflammatory signaling
- Autonomic Imbalance: Promotes parasympathetic dominance
- Network Homeostasis: Reorganizes whole-brain connectivity
Participant Profile
The cohort represented a treatment-experienced, chronically ill population:
- 75% suffered migraines ≥10 years (range: 1-55 years)
- Mean baseline: ~13 migraine days/month
- Average pain intensity: 7.85/10 (65% in severe range)
- 90% used prescription medications and complementary therapies
- Common triggers: stress/anxiety (95%), bright lights (80%), hormonal changes (75%)
- Prevalent symptoms: throbbing pain, photophobia, phonophobia, difficulty concentrating
Primary Outcomes
Results demonstrated rapid, multidimensional improvements with large effect sizes:
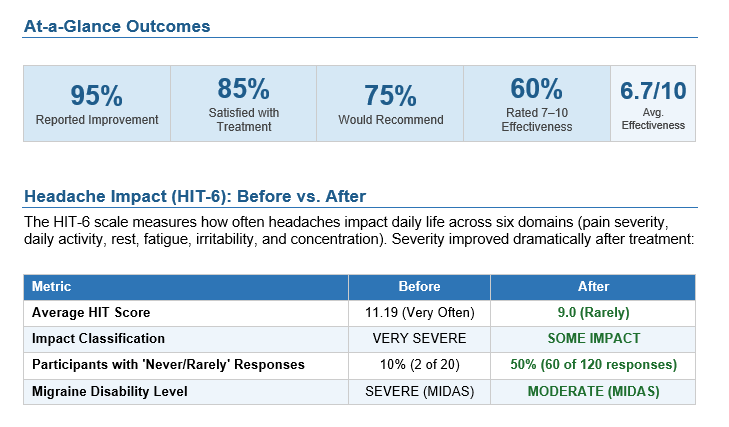
MIDAS (Migraine Disability Assessment):
- Scores declined from 77.7 (Severe Disability) to 16.5 (Moderate Disability)
- Represents 79% reduction in migraine-related disability
HIT-6 (Headache Impact Test):
- Scores decreased from 67.15 ("Very Severe Impact") to 53.95 ("Some Impact")
- Categorical shift in functional impact
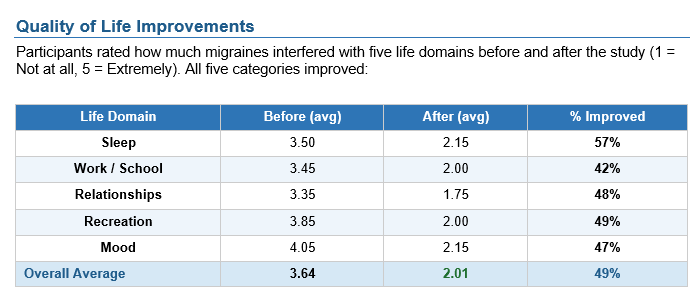
Quality of Life:
- 49% overall improvement across five domains
- Sleep: 57% improvement (3.5 → 2.15)
- Work/School: 42% improvement (3.45 → 2.0)
- Relationships: 48% improvement (3.35 → 1.75)
- Recreation: 49% improvement (3.85 → 2.0)
- Mood: 47% improvement (4.05 → 2.15)
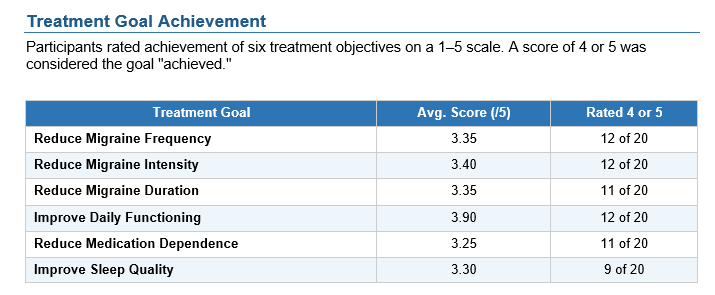
Treatment Goals:
- 56% of all participant-defined goals rated as "mostly" or "completely" achieved
- Mean overall effectiveness rating: 6.7/10
- 60% rated effectiveness ≥7/10
90-Day Follow-Up Findings
Nine participants (45% response rate) completed voluntary follow-up assessments revealing sustained benefits
- 89% reported less frequent migraines versus baseline
- 78% reported reduced intensity and painfulness
- 78% experienced only 0-2 migraine days in final three weeks
- Pain severity remained in mild-to-moderate range (1-6/10)
- No respondents reported severe pain (7-10/10)
- 89% satisfied or very satisfied with treatment
- No moderate or severe delayed adverse events

Safety Profile
NGBBMP demonstrated excellent tolerability:
- No serious adverse events across all 100 sessions
- Minimal side effects (occasional mild, transient headache)
- Signals delivered at ~2.5 picowatts (1/10,000th power of AA battery)
- Non-invasive, passive, drug-free intervention
- No contraindications with existing medications
Clinical Significance
The findings are particularly noteworthy given the treatment-resistant nature of the cohort and the brevity of intervention. Unlike preventive medications requiring weeks to months for effect, many participants reported benefits after the first session, with substantial improvements within four weeks. The passive nature eliminates barriers associated with cognitive demand, making it accessible for individuals unable to engage in traditional neurofeedback.
Qualitative reports reinforced quantitative findings, with participants describing longest migraine-free periods in years, improved sleep architecture, enhanced emotional regulation, reduced trigger sensitivity, and decreased medication reliance.
Study Limitations
As an uncontrolled feasibility study, limitations include: small sample size (n=20), absence of randomization or sham condition, reliance on self-report measures, brief intervention window, and limited follow-up response rate (45%). Future randomized, double-blind, placebo-controlled trials incorporating objective biomarkers (qEEG, fMRI, HRV) and extended follow-up are essential to establish causality and durability.
Broader Implications
This study provides proof-of-concept evidence supporting NGBBMP as a rapid, safe, well-tolerated intervention producing meaningful reductions in migraine burden. The mechanisms align with migraine pathophysiology involving network dysregulation, suggesting potential applications beyond migraine to chronic pain syndromes, PTSD, post-concussion syndrome, sleep disorders, and cognitive dysfunction—conditions sharing overlapping neural network disturbances.
With an estimated 30,000 sessions delivered since 2020 without notable adverse effects, and preliminary VA-funded research underway examining neurophysiological changes via resting-state MRI, the platform represents a promising addition to the neurotherapeutic armamentarium—particularly for individuals seeking non-pharmacologic, accessible, and patient-centered care alternatives.

Recent Posts